Topics
Table of Contents
Rare but potentially dangerous arterial anomalies, Arteriovenous Malformations (AVMs) can impact the brain, spine, or other body organs. Many people don’t know they have an AVM until symptoms start to show up. Patients can seek prompt medical attention and avoid difficulties by being aware of Arteriovenous Malformations, what they are, why they happen, and how to manage them.
For patients and carers, this guide provides a straightforward explanation of Arteriovenous Malformations.
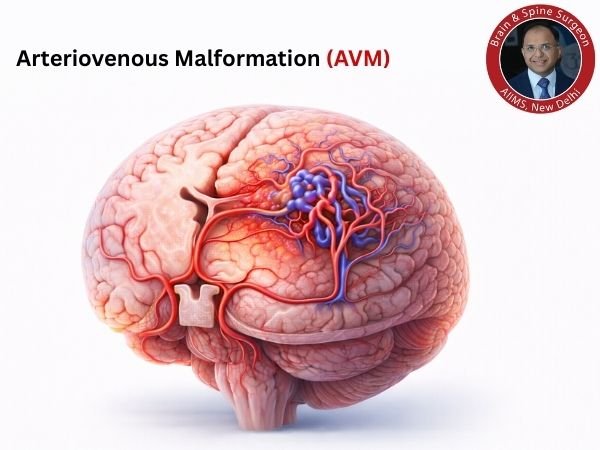

An Arteriovenous Malformation: What Is It?
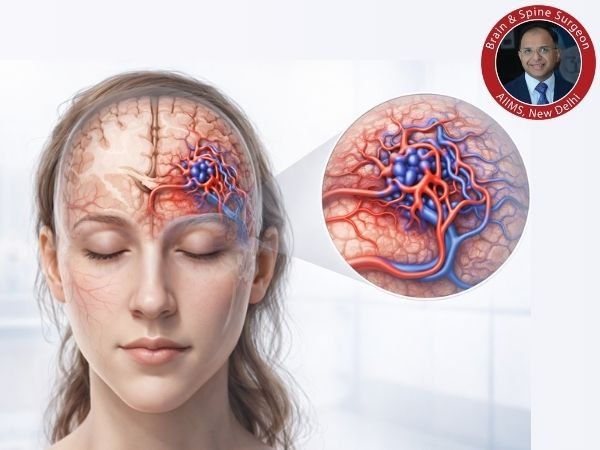
An unusual tangle of blood vessels where arteries join directly to veins without the typical network of small capillaries in between is known as an Arteriovenous Malformation (AVM).
Typical blood flow
The heart’s oxygen-rich blood is transported by arteries.
Capillaries facilitate the exchange of oxygen while slowing blood flow.
Blood is returned to the heart via the veins.
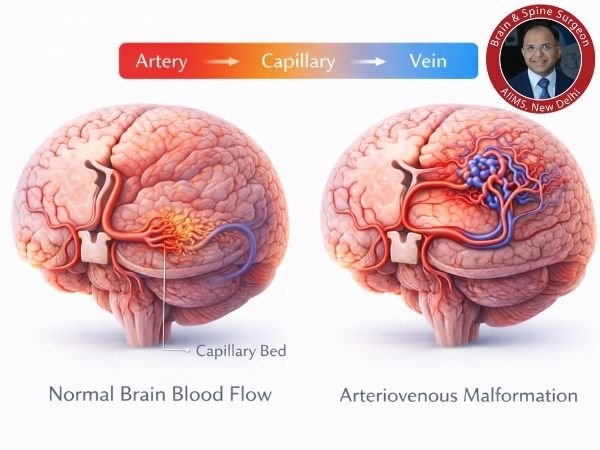

Within AVM
Veins and arteries are directly connected.
Blood moves too quickly.
Tissues nearby might not receive adequate oxygen.
Vessel walls deteriorate and are more likely to burst.
Because it can result in brain haemorrhage, the most serious kind is Brain AVM (cerebral AVM).
Arteriovenous Malformation Types
AVMs can develop in several body areas, including:
1. AVM of the brain (cerebral AVM)
Most prevalent and most hazardous
May result in brain haemorrhage or stroke.
May result in seizures.
2. AVM in the spine
Takes place within or around the spinal cord.
May result in paralysis or weakness.
Can have an impact on bowel and bladder control.
3. AVM in the periphery
Takes place in the lungs, limbs, or other organs.
May result in skin changes, discomfort, or swelling.

Arteriovenous Malformation Causes
AVMs are typically:
Congenital, meaning it exists from birth
Grow when the foetal blood vessels are forming.
Not typically inherited
Uncommon genetic correlations
- AVM risk is increased by certain circumstances, including:
- Hemorrhagic telangiectasia inherited (HHT)
- Important: A lot of patients have no known cause.
- AVM Symptoms
The location and size of the AVM determine the symptoms.
Typical AVM Symptoms in the Brain
- A sudden, intense headache
- Seizures
- Arm or leg weakness
- Speaking difficulties
- Vision issues
- Feeling numb or tingly
- Issues with balance
AVM Rupture Warning Signs (Medical Emergency)
- The “worst headache of life” all at once
- Throwing up
- Unconsciousness
- Abrupt neurological impairment
If any of these happen, get emergency care right away.
Arteriovenous Malformation Complications
AVMs can cause major issues if left untreated:
- Brain haemorrhage, or brain bleeding
- A stroke
- Progressively worsening neurological impairments
- Prolonged headaches
- Disorders of seizures
- Burden on the heart (in large AVMs)
The most severe consequence is brain haemorrhage.
How Do They Diagnose AVMs?
Results are greatly improved by early diagnosis.
1. CT scan
Rapid identification of cerebral haemorrhage
In an emergency, the initial test is frequently
2. Brain MRI
- An in-depth look into the AVM structure
- Aids in the planning of treatment
3. CT Angiography (CTA)
Displays the anatomy of blood vessels.
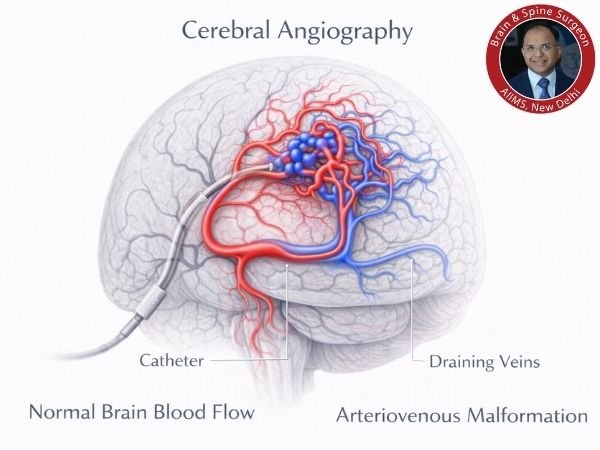
4. The Gold Standard of Digital Subtraction Angiography (DSA)
- The most accurate test
- Maps that show veins draining and arteries feeding
- Necessary prior to therapy
Spetzler-Martin Grading or AVM Grading
In order to evaluate surgical risk, doctors grade brain AVMs according to:
- The AVM’s size
- Where in the brain
- Pattern of venous drainage
Grades I through V are available:
- Grade I–II: Reduced risk of surgery
- Grade III: Moderate danger
- Grade IV–V: Higher risk; frequently treated with radiosurgery or conservative measures
Related Post: Draining Vein Shielding During Gamma Knife Radiosurgery in Intracranial Arteriovenous Malformations
Arteriovenous Malformation Treatment
Each patient receives individualised treatment. Not every AVM needs surgery right away.
Factors Influencing the Choice of Treatment
- Age of the patient
- AVM placement and size
- Bleeding history
- Signs and symptoms
- General well-being
1. Conservative Administration ( Important Observation )
Suggested when:
- AVM is asymptomatic and tiny.
- The danger of surgery is considerable.
- The patient is elderly.
Consists of:
- Frequent follow-up MRI
- Medication for seizure control
- Control of blood pressure
2. AVM Surgery, or Microsurgical Removal
For many accessible brain AVMs, this is the best choice.
Benefits
Cure right away if totally removed
Reduces the chance of bleeding in the future
When advised:
- Poor quality AVMs
- Previous bleeding
- A site that is easily accessible
3. Embolisation of the Endovascular
A minimally invasive technique in which medical professionals:
Put a catheter into your groin.
To plug aberrant vessels, inject a substance that resembles glue.
Opportunities
- Frequently carried out prior to surgery
- Occasionally, when used alone
- Decreases blood flow and AVM size
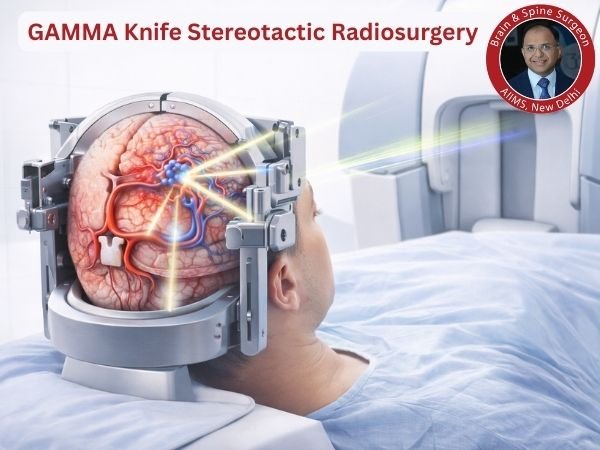
4. Gamma Knife stereotactic radiosurgery
Gradually closes the AVM using concentrated radiation.
Ideal for:
AVMs that are little to medium
High-risk or deep surgical sites
Critical information:
Two to three years are needed for total obliteration.
There is still a slight chance of bleeding at this time.

Rehabilitation Following AVM Therapy
The sort of treatment determines recovery.
Following Surgery
- Typical length of hospital stay: 3–7 days
- Gradual return to regular activities
- Imaging follow-up is necessary.
Following Radiosurgery
Typically, outpatient
Frequent follow-up MRI
AVM closure over time, gradually
Rehabilitation could consist of:
- Physical therapy
- Speech therapy
- Management of seizures
When Is the Right Time to See a Neurosurgeon?
Seek advice from an expert if you encounter:
- Unknown seizures
- Frequent, intense headaches
- Unexpected neurological symptoms
- Unexpected AVM discovered during scan
- Vascular malformations in the family history
Early professional assessment can save lives.
Lifestyle Advice for People Living With an AVM
Individuals with an AVM diagnosis should:
- Keep your blood pressure under control.
- Don’t smoke.
- Avoid drinking too much alcohol.
- Regularly use anti-seizure medications, if prescribed.
- Attend the follow-ups as planned.
- Seek emergency attention if you have a sudden, intense headache.

Important Takeaways
- An aberrant artery-vein connection is known as an Arteriovenous Malformation.
- Brain AVMs may result in convulsions, stroke, or bleeding.
- Many AVMs are identified by accident and are congenital.
- The gold standard for diagnosis is Digital Subtraction Angiography (DSA).
- Surgery, embolisation, radiosurgery, and observation are available treatment options.
- Results are considerably improved by early specialist review.
FAQ’s
1. Is AVM a tumour of the brain?
No, a tumour is not an AVM. It is an irregular blood vascular connection.
2. Can AVM disappear by itself?
Very infrequently. The majority of AVMs are persistent and need to be treated or monitored.
3. What is the chance of rupturing an AVM?
Generally speaking:
2-4% annually for cerebral AVMs
If it has already bled, the risk is increased.
4. Does AVM run in families?
Generally speaking, no. The majority of AVMs happen infrequently. The proportion associated with hereditary diseases such as HHT is quite low.
5. Is it possible to heal AVM?
Indeed, a lot of AVMs can be fully healed using:
Microsurgery
Radiosurgery
or a combination of therapies
The location and AVM grade determine the outcome.
6. How risky is AVM surgery?
There are hazards, just like with any brain operation. However, surgery can be extremely safe and curative in skilled hands and in circumstances that are carefully chosen.
7. Can seizures be brought on by AVM?
Indeed, one of the most typical initial signs of brain AVM is seizures.
Sources:
- https://www.ncbi.nlm.nih.gov/books/NBK430744/
- https://pubmed.ncbi.nlm.nih.gov/25241099/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC8396465/
- https://www.ncbi.nlm.nih.gov/books/NBK531479/
- https://pubmed.ncbi.nlm.nih.gov/33004601/
- https://www.ninds.nih.gov/health-information/disorders/arteriovenous-malformations-avms
- https://pubmed.ncbi.nlm.nih.gov/11897302/