Topics
Table of Contents
Injuries to the lumbar spine can change a person’s life, particularly if they involve burst fractures, in which the vertebral body fractures and shards disperse in all directions. The transpedicular approach, a minimally invasive but potent technique for stabilising the spine and decompressing nerves, is one of the most successful methods of modern spine surgery.
Everything a patient (or carer) needs to know about lumbar burst fractures and their surgical treatment is covered in this guide.
A Lumbar Burst Fracture: What is it?
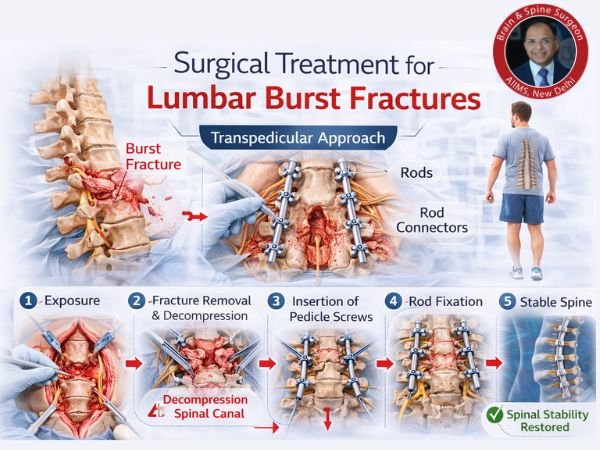
When a vertebra in the lower back (lumbar spine) fractures as a result of high-energy trauma, such as:
-
Traffic accidents on roads
-
Falls from a height
-
Sports-related injuries
In contrast to straightforward compression fractures, burst fractures include:
-
Collapse of the spinal column
-
Parts that are projecting into the spinal canal
-
Possible compression of the spinal cord or nerves
As a result, they become more serious and frequently call for surgery.
A Lumbar Burst Fracture: How Serious Is It?
The severity is determined by:
-
Spinal canal compromise severity
-
Injury to the spinal cord or nerves
-
Instability of the spine
In extreme circumstances, patients may encounter:
-
Paralysis or weakness
-
Sensation loss
-
Bowel or bladder dysfunction
According to studies, burst fractures can seriously impair the spinal canal (up to about 60%), so prompt treatment is essential to avoid irreversible brain damage.
Therapy for Spinal Burst Fractures
The degree of the fracture determines the treatment:
1. Non-Surgical Care
-
Bracing
-
Pain control
-
Short-term bed rest
-
Physical therapy
Used exclusively when:
-
No neurological impairment
-
Stable fracture
2. Surgery (When Required)
It is advised to have surgery if:
-
Nerve compression is present
-
The spine is not stable
-
There is a severe malformation (kyphosis)
Common surgical objectives
-
Relax your nerves
-
Maintain spinal stability
-
Restore the alignment and height of the vertebrae
Lumbar Vertebral Burst Fractures: Transpedicular Surgery
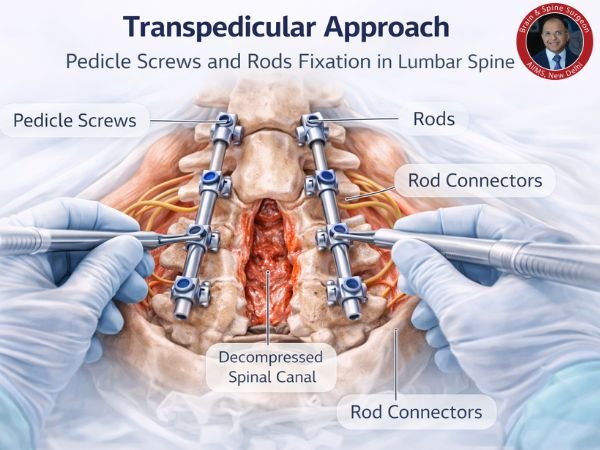
The Transpedicular Approach: What Is It?
Through the pedicles, or bony bridges of the vertebra, the surgeon can access the fractured vertebra using the transpedicular approach, a posterior (from the rear) surgical procedure.
It permits:
-
Removal of nerve-compressing bone pieces
-
Installing rods and screws to provide stability
-
Reconstruction of the spinal column
How the Process Operates
-
A tiny cut on the back
-
Inserting pedicle screws into neighbouring vertebrae
-
Access obtained by pedicle
-
Removal of broken bones (decompression)
-
Inserting a cage or bone graft (if necessary)
-
Rods that support the spine
Transpedicular Surgery Benefits
-
One posterior approach (no anterior surgery required)
-
Less intrusive than conventional techniques
-
Effective decompression of the spinal canal
-
Robust stability with pedicle screws
-
Shorter hospital stays and quicker recovery
Clinical research demonstrates
-
Neurological improvement in about 70–77% of patients
-
Significant spinal deformity correction
-
High rates of fusion (~90%+)
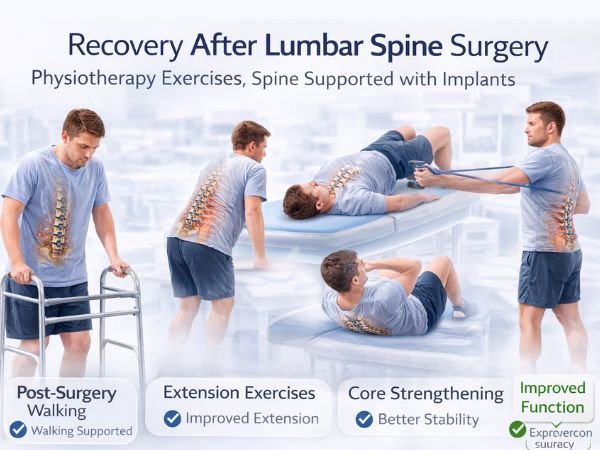
Recuperation Following Lumbar Spine Surgery
The degree of an injury and general health have an impact on recovery.
Quick Recuperation
-
Hospital stay: around three to seven days
-
Early pain alleviation
-
In a few days, walking with assistance
Temporary (0–6 Weeks)
-
Restricted lifting and bending
-
Gradual mobilisation
-
Physiotherapy begins
Extended (3–6 Months)
-
Go back to your regular activities
-
Strengthening of muscles
-
Near-normal movement
Complete Recuperation
Usually, six to twelve months
Success Rate of Spine Fracture Surgery
Excellent results have been demonstrated by modern surgical procedures, particularly transpedicular fixation:
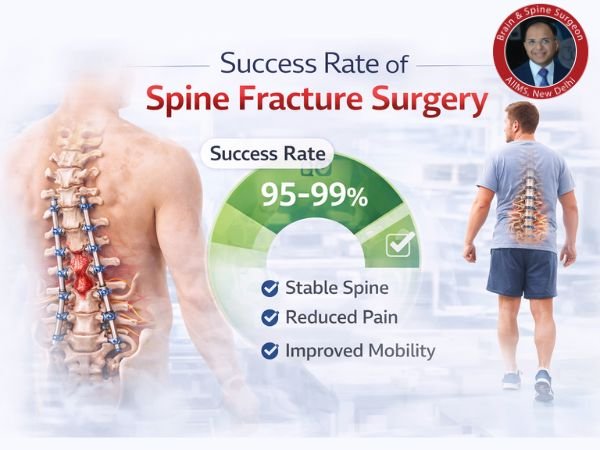
-
High rates of fusion (~90%)
-
Significant decrease in pain
-
Restoration of alignment and height of the vertebrae
-
Most patients experience neurological recovery
However, results rely on:
-
When to perform surgery
-
The degree of nerve damage
-
Age and bone condition of the patient
Hazards and Difficulties
As with any operation, there are risks to consider:
-
An infection
-
Bleeding
-
Implant failure (particularly osteoporotic bone)
-
Neurological healing that is not full
These dangers are greatly decreased by selecting a skilled neurosurgeon.
In conclusion
Lumbar burst fractures are dangerous injuries that need to be treated quickly and professionally. By providing a safe, efficient, and minimally invasive method for nerve decompression and spinal stabilisation, the transpedicular technique has transformed treatment.
Most patients can anticipate substantial pain reduction, increased mobility, and a high quality of life following surgery thanks to improvements in surgical methods and post-operative care.
FAQ’s
1. Is surgery necessary for the healing of a lumbar burst fracture?
Yes, provided that there is no nerve injury and it is stable. However, surgery is typically necessary for unstable fractures.
2. Is it safe to perform transpedicular surgery?
Indeed. When done by skilled surgeons, it is commonly utilised and regarded as safe with positive results.
3. After surgery, will I be able to walk again?
Mobility is restored for many people, particularly if surgery is performed early. Each patient has a different neurological recovery.
4. What is the duration of the procedure?
Depending on complexity, it usually takes two to four hours.
5. Will implants last a lifetime?
Yes, most of the time. They are intended to stay in place unless something goes wrong.
6. Does the procedure hurt?
With medicine, post-operative pain can be controlled and gets better in a few days.
7. When will I be able to go back to work?
-
Desk work: four to six weeks
-
Physical work: three to six months
Sources: