Topics
Table of Contents
A rare but dangerous medical emergency is a subdural haematoma without trauma, particularly among haemophiliacs. Spontaneous bleeding is more dangerous since it can happen without a clear cause, in contrast to usual brain bleeds caused on by head trauma.
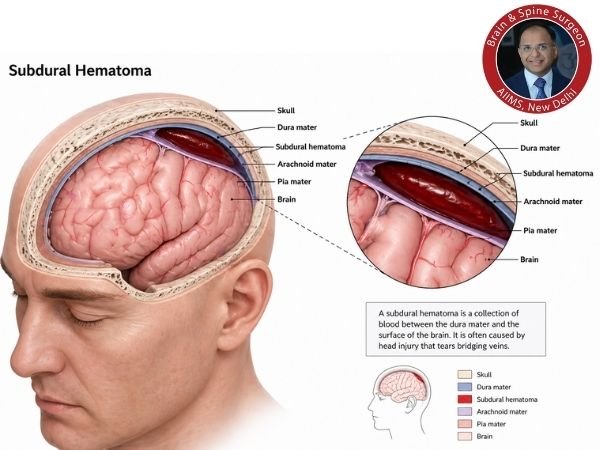

Even mild internal bleeding in haemophiliac patients can quickly develop into potentially fatal consequences including spontaneous subdural haematomas, a form of intracranial haemorrhage.
Everything a you need to know is included in this guide, from causes and symptoms to preventive and emergency care.
A subdural haematoma: what is it?
A Spontaneous Subdural Hematoma in Hemophilia occurs when blood builds up between the dura, the outer layer of the brain, and the brain’s surface. Neurological symptoms result from this accumulation, which puts more strain on the brain.
Types:
- Acute: develops quickly and is frequently fatal
- Subacute: symptoms take days to manifest
- Chronic: takes weeks to develop
Even a spontaneous (non-traumatic) bleed might result in rapid deterioration in haemophilia patients.
Why Does Haemophilia Increase the Risk of Brain Bleeding?
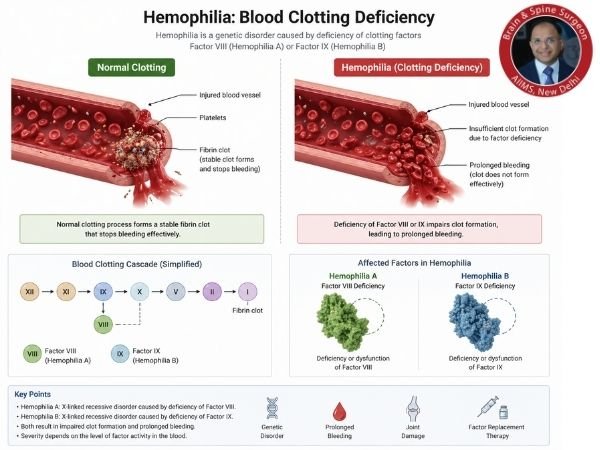

A genetic condition known as haemophilia causes the blood to lack vital clotting proteins (Factor VIII or IX). This results in:
- Extended bleeding
- Inability to form clots
- A higher chance of internal bleeding
Why Is the Brain in Danger?
- Blood vessels that are brittle may burst on their own
- Significant bleeding can result from minor, undetected wounds
- Bleeding is made worse by delayed clot formation
The danger of haemophilia brain haemorrhage is greatly increased by this, particularly for intracranial problems.
Related Post: Cerebrovascular Diseases: Symptoms, Causes, Treatment & Prevention
Reasons for Haemophiliac Spontaneous Subdural Haematoma
Although trauma is the most frequent cause in the general population, haemophiliacs may experience subdural haematomas in the absence of trauma for the following reasons:
1. Deficiency in Coagulation
- Uncontrolled bleeding results from a lack of clotting factors.
2. Unnoticed or Minimal Injury
- Bleeding can occur from even small bumps.
3. Abrupt Rise in Blood Pressure
- Can cause tiny cerebral veins to burst.
4. Using blood thinners
- Drugs may make bleeding more likely.
5. Severe haemophilia
- The most vulnerable patients are those with extremely low clotting factor levels.
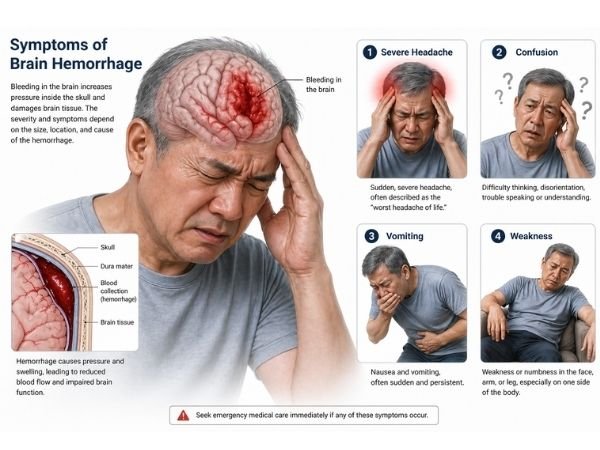
Early Warning Signs of Intracranial Haemorrhage
Early detection of cerebral haemorrhage symptoms can save lives.
Typical Symptoms:
- Severe or ongoing headache
- Throwing up
- Confusion or drowsiness
- Slurred speech
- Arm or leg weakness
- Seizures
- Lack of awareness
Emergency Red Flags:
- Abrupt decline in awareness
- Unequal pupils
- Frequent vomiting
- Unknown reason of a severe headache
These symptoms indicate a brain bleed that has to be treated immediately.
Diagnosis
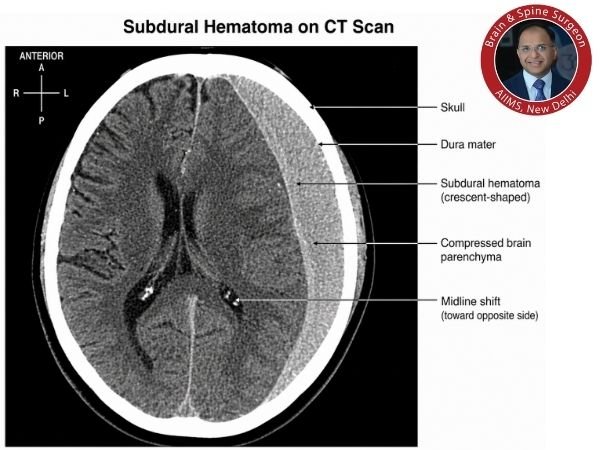

In such situations, prompt diagnosis is crucial.
Important Research:
- First-line imaging with a CT scan of the head
- MRI Brain: a thorough evaluation
- Blood tests to assess levels of clotting factor
In situations of Spontaneous Subdural Hematoma in Hemophilia, early imaging aids in confirmation.
Emergency Brain Bleeding Treatment

In haemophilia, a Spontaneous Subdural Hematoma in Hemophilia is a neurosurgical emergency.
1. Quick Factor Replacement
- Haemophilia A, or Factor VIII
- Haemophilia B, or Factor IX
- Restores the capacity to clot and regulates bleeding
2. Stabilisation of Healthcare
- ICU surveillance
- Regulation of intracranial pressure
- Preventing seizures
3. Surgical Procedure
In extreme circumstances, necessary:
- Drainage from burr holes
- Craniotomy (clot removal)
4. Assistance/Supportive Care
- Treatment with oxygen
- Fluid control
- Neurological surveillance
Survival and results are greatly enhanced by early treatment.
Problems if Untreated
Treatment delays may result in:
- Irreversible brain damage
- Paralysis
- Impaired cognitive function
- Coma
- Death
This emphasises how critical it is to identify cerebral haemorrhage signs as soon as possible.
Related Source: Watch this video for “Head Injury” explanation by Dr. Deepak Agrawal (AIIMS Prof. Neurosurgeon)
VIDEO Sources
Preventive Techniques for People with Haemophilia
1. Frequent Factor Treatment
Prophylactic (preventive) replacement of coagulation factors
2. Stay away from high-risk activities
Reduce the likelihood of a head injury
Realted Post: Head Injury – Decompressive Craniectomy
3. Regular Observation
Frequent consultations with a professional
4. Prompt Medical Care
Even for minor neurological symptoms or headaches
5. Teaching Carers
Early detection saves lives
When would you see a Physician?
Seek medical attention right away if a patient with haemophilia experiences:
- Abrupt, intense headache
- Confusion or vomiting
- Any symptom related to the nervous system
- Even a small head injury
Never disregard symptoms; prompt intervention is essential.
Conclusion
In haemophilia, Spontaneous Subdural Hematoma in Hemophilia is an uncommon but potentially fatal disorder that needs to be treated right away. Lives can be saved by being aware of the danger of haemophilia brain bleeding, identifying the signs of cerebral haemorrhage, and getting emergency care for a brain bleed.
The key elements of treating this serious illness continue to be early diagnosis, timely treatment, and preventive care.
FAQ’s
Can a subdural haematoma develop in the absence of trauma?
Yes, particularly in haemophiliacs who may experience spontaneous bleeding as a result of clotting abnormalities.
What makes haemophilia a risk factor for brain haemorrhage?
Even minor bleeding can prove fatal due to improper blood clotting.
What are a brain bleed’s initial symptoms?
Early warning indications include weakness, disorientation, vomiting, and a severe headache.
Can a spontaneous subdural haematoma be treated?
Yes, with prompt surgical intervention if necessary, early diagnosis, and factor replacement.
How quickly should therapy start?
Right away. Delays in treating a brain bleed can be lethal, making it a medical emergency.
Is it avoidable?
Regular factor therapy and early symptom diagnosis significantly lower risk, albeit they are not entirely prevented.
Sources:
- https://pmc.ncbi.nlm.nih.gov/articles/PMC11925473/
- https://pubmed.ncbi.nlm.nih.gov/12865541/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC7398207/
- https://pubmed.ncbi.nlm.nih.gov/35273899/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC5094152/
- https://wjarr.com/sites/default/files/fulltext_pdf/WJARR-2024-1693.pdf
- https://pmc.ncbi.nlm.nih.gov/articles/PMC4603318/
- https://pubmed.ncbi.nlm.nih.gov/31562972/